

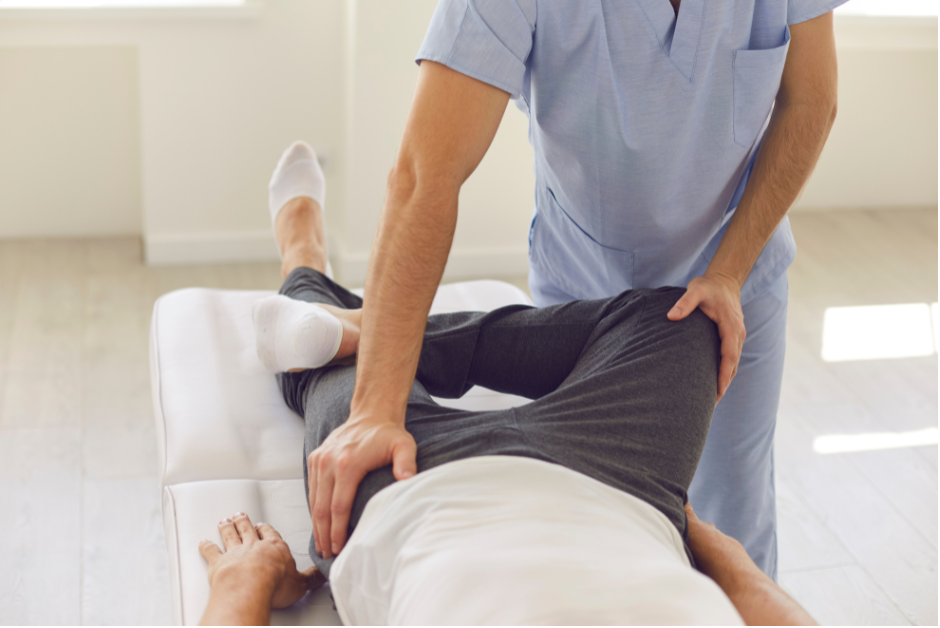
We offer Male Pelvic Floor Therapy to help men experiencing pelvic pain, urinary or bowel issues, or sexual dysfunction. Our trained physiotherapist provide private, one-on-one sessions focused on restoring pelvic floor muscle function, improving control, and enhancing overall quality of life.
The pelvic floor is a group of muscles that support the bladder, bowel, and reproductive organs.
When these muscles become weak, tight, or uncoordinated, they can lead to a range of symptoms, including:
Pelvic floor dysfunction can affect men of all ages — and it’s both common and treatable with the right therapy.
Professional, evidence-based, and discreet approach to men’s pelvic health. Your treatment begins with a comprehensive assessment to understand your symptoms, medical history, and muscle function.
Your personalized plan may include:
All sessions are conducted in a private and supportive environment, ensuring comfort and confidentiality throughout your care.
Here is a typical flow of what you might expect at your first visit, and what treatment sessions may include.
Initial Assessment (First Visit)
1 Medical History & Symptom Discussion
The therapist will ask detailed questions about your symptoms: urinary habits (incontinence, urgency, frequency), bowel habits (constipation, straining, leakage), sexual function (erections, ejaculation, pain), pain in the pelvic, perineal, rectal, testicular or lower-back/hip region.
They’ll ask about surgeries (especially prostate surgery or radiation), trauma, lifestyle factors (heavy lifting, sitting time, exercise), posture/breathing patterns, hip/spine/back problems and other contributing factors.
The therapist will explain what pelvic floor physiotherapy is, how it works, what to expect, your rights (consent, comfort, decline internal exam) and answer any questions you have.
2 Physical/Orthopaedic Screening
The therapist will assess your posture, how you move (walking, squatting, lifting), hip/back/spine range of motion, strength of surrounding muscles (glutes, hips, abdomen, back). Dysfunction in these areas often contributes to pelvic floor problems.
They may assess breathing pattern (diaphragm function), core activation and how your body handles pressure (e.g., when you cough or lift).
They may examine external pelvic region (perineum, testicular/testes area, external anal area) for muscle tightness, trigger points, tenderness, tone.
3 Pelvic Floor Muscle Assessment
With your informed consent, an internal rectal (in men) pelvic floor muscle assessment may be offered. This helps assess muscle resting tone, contractile ability, coordination (can you both contract and release?), pain or trigger points in the muscles.
The therapist explains exactly how it will happen, what you need to do (e.g., lie on side or stomach, cover yourself, they leave the room while you change) and you can decline or defer the internal exam.
The internal exam may include asking you to contract (like stopping urine/gas) and to bear down (push like a bowel motion) to assess muscle control both ways (strength & relaxation).
4 Feedback & Initial Treatment Plan
After the assessment, the therapist explains their findings: what seems to be contributing, what your goals are, what the treatment plan might look like (sessions frequency, home-exercise requirements, expected timeline).
In many cases, treatment begins immediately: manual therapy for muscle tightness, introduction to breathing and core exercises, posture correction, early home-program.
Recovery varies widely depending on the individual, the severity and duration of the problem, whether there are underlying surgical/nerve issues, and how consistent you are with home-programming. Here’s a general guide:
While many men benefit significantly from pelvic floor physiotherapy, there are reasons why progress may be slower or outcomes may be limited:
Male pelvic floor physiotherapy is a safe, evidenced-based, and increasingly recognised treatment pathway for men experiencing bladder, bowel, sexual or pelvic pain issues. With a comprehensive assessment, skilled treatment, and your commitment to the home-program and lifestyle change, many men experience meaningful improvement. The journey may require patience, but you are in control of your healing process — and you deserve to reclaim comfort, function and confidence.
Our priority is your health. We understand that everybody, every injury and every recovery journey is different. We guarantee to provide you with the best possible care with all the time and efforts you deserve.
Monday : 7:00 AM – 8:00 PM
Tuesday : 7:00 AM – 8:00 PM
Wednesday : 7:00 AM – 8:00 PM
Thursday : 7:00 AM – 8:00 PM
Friday : 7:00 AM – 8:00 PM
Saturday : 10:00 AM – 3:00 PM
Sunday : Closed
Our priority is your health. We understand that everybody, every injury and every recovery journey is different. We guarantee to provide you with the best possible care with all the time and efforts you deserve.